
Tag: TMJ pain
16 Posts


Patient presenting Oromandibular Dystonia two years after the first consultation, when she presented temporomandibular disorder without dystonia. Oromandibular dystonia and the connection with cranio-cervico-mandibular disorders.

High technology in the diagnosis and treatment of TMJ pathologies and the optimized bite for enhance the highest performance in Sports Dentistry

Posteriorization of the Mandibular Condyle, Compression of the Retrodiscal Tissue and Anteriorization of the Articular Disc as a cause of Neurologic Pain. Recovery of the Physiological Relationship of the Head of the Mandible with the Articular Disc. Series of clinical cases.

Treatment of TMJ Pathologies: Patient with headache and excessive clenching. Physiological Neuromuscular Rehabilitation. First and second phase. Case Report.

TMJ Pathology in Professional Musicians: A look beyond the risk factors. Physiological Neuromuscular Rehabilitation. First and second phase. Case Report.
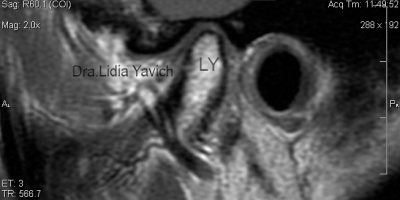
TMJ Pathologies Treatment: Patient with headache for 30 years. Neuromuscular Physiological Rehabilitation. First and second phase. Case Report.
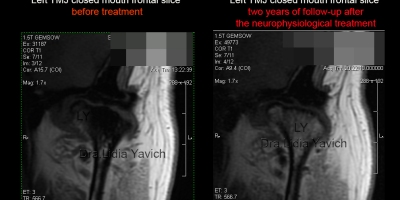
Reestablishment of the Bone Marrow Signal in a case of Avascular Necrosis of the Mandibular Head. Monitoring two years after treatment.

Temporomandibular Joint Pathology in a Patient with Congenital Fusion of two Cervical Vertebrae. First and Second Phase. Case Report.
